Increasing bone strength with food: Nutritionist Sarah Di Lorenzo’s advice on what to eat
Bone density loss is silent and painless — until something breaks.
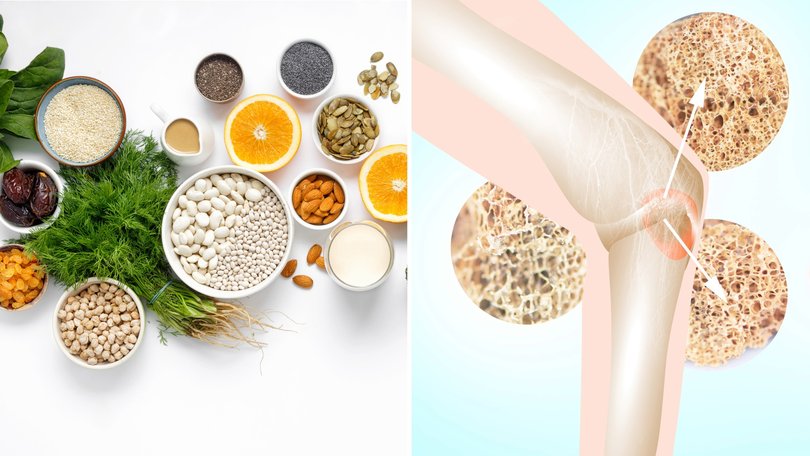
Your skeleton is far more than just a structural frame. Bones are a living, metabolically active, tissue that are constantly being broken down and rebuilt throughout your life.
What makes bone loss so dangerous is that it is completely silent and painless until something breaks. There are no warning symptoms as your bone density quietly declines over years or decades.
This is why osteoporosis is called a “silent disease” and why prevention is the only truly effective strategy.
Sign up to The Nightly's newsletters.
Get the first look at the digital newspaper, curated daily stories and breaking headlines delivered to your inbox.
By continuing you agree to our Terms and Privacy Policy.Beyond structure, bones produce blood cells in the marrow, store 99 per cent of the body’s calcium, and regulate heart rhythm, nerve function, and muscle contraction.
This makes the status of your bones central to your overall health in ways most people never consider.
Bone density peaks around age 25 to 30. From then on it moves from building to maintaining. The higher your peak bone mass, the greater your reserve before crossing into osteoporosis territory.
Strong bones give you the freedom to move, stay active, and remain independent well into old age. Taking care of bone health should be a priority that rarely gets the attention it deserves until it is too late. What you eat can play a big role in bone strength.
Our first thoughts about the best foods for bone health would be straight to calcium and dairy. And while calcium absolutely matters, bone strength is built on a far richer nutritional foundation than a glass of milk can provide.
As a nutritionist, what I see time and again is that people are unknowingly undermining their bones through what they’re not eating — and what they are.
Calcium is the primary mineral in bone tissue, making up roughly 70 per cent of bone’s dry weight.
Adults need around 1000–1200mg daily, and that demand increases after menopause when bone loss accelerates.
The best food sources are dairy (milk, yoghurt, cheese), canned fish with edible bones (sardines, salmon), almonds, tahini, and leafy greens like bok choy and kale.
But here’s the catch, and this is what many people forget, calcium cannot do its job without the right co-factors to absorb it and direct it into bone tissue.
Vitamin D is key for calcium absorption. Without sufficient vitamin D, the body absorbs as little as 10–15 per cent of the calcium you consume. With optimal vitamin D levels, that absorption jumps to 30–40 per cent.
Vitamin D is produced in the skin from sunlight exposure, but in practice most adults, particularly in office environments or cooler climates, are chronically deficient.
Dietary sources include oily fish, egg yolks, and fortified foods, but food alone rarely provides enough.
A blood test (25-hydroxy vitamin D) will tell you what your Vitamin D levels are and most people benefit from supplementation, particularly during winter months.
Vitamin K2 is your body’s bone director. It is the nutrient most people have never heard of, yet it’s one of the most critical for bone health.
Vitamin K2 activates a protein called osteocalcin, which literally carries calcium into bone tissue and binds it there.
Without K2, calcium absorbed into the bloodstream can end up deposited in soft tissues and arteries rather than in your bones and this is what you don’t want. The best dietary sources of K2 are fermented foods, cheese, egg yolks, and grass-fed butter.
Protein is the scaffold your bones need. Bone is not just mineral, it is approximately 30 per cent collagen protein, which provides the flexible scaffold that gives bone its ability to resist fracture rather than simply shatter.
Inadequate protein intake is directly associated with lower bone mineral density and higher fracture risk.
You should aim for at least 1.2-1.6g of protein per kilogram of body weight daily from quality sources such as eggs, fish, chicken, meat, Greek yoghurt, legumes and quality protein powders.
Magnesium, zinc and collagen are the co-factors. Magnesium is involved in over 300 enzymatic reactions, including bone mineralisation.
Around 60 per cent of the body’s magnesium is stored in bone itself. Good sources include pumpkin seeds, dark leafy greens, dark chocolate, and legumes. Zinc supports the bone-building cells (osteoblasts) and helps with collagen synthesis; you can find it in meat, shellfish, and pumpkin seeds. Vitamin C is essential for collagen production so make sure to prioritise berries, citrus, capsicum, and kiwifruit.
Just as important as what you add is what you reduce.
Excessive sodium leaches calcium from the body through urine. High alcohol intake impairs bone-building cell activity and reduces calcium absorption.
Excess caffeine (more than 3–4 cups daily) can also accelerate urinary calcium loss. A high intake of soft drinks, especially cola has been linked to lower bone density, likely due to phosphoric acid disrupting calcium balance.
A true bone health wholistic approach would bring together a nutrient-dense diet rich in calcium, vitamin D, vitamin K2, magnesium, and protein, alongside regular weight-bearing and resistance exercise, healthy sleep, stress management, and minimising the dietary and lifestyle factors that silently leach minerals from bone over time.

